|
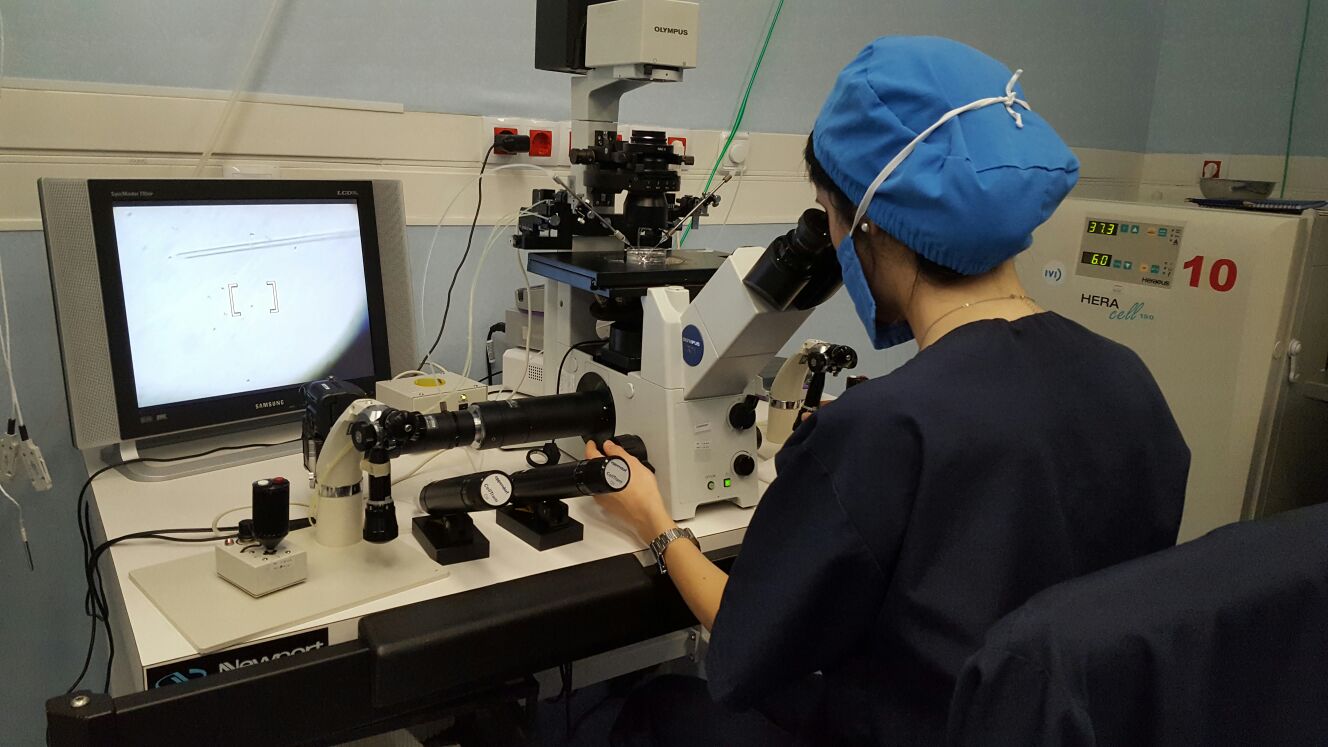
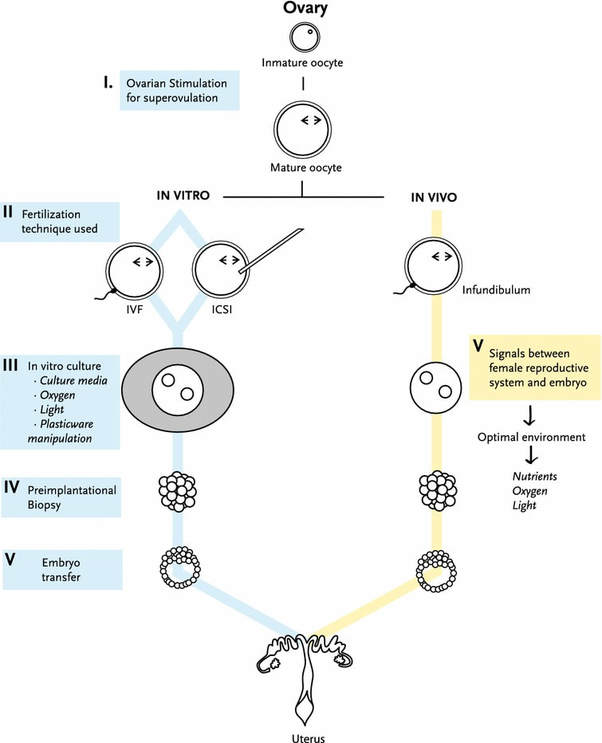
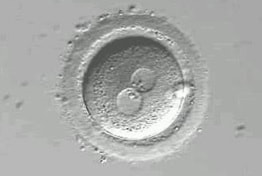
Author: Belén Gómez Giménez "It is without question that embryologists work tirelessly to help families achieve their dream of bringing a healthy baby home". It is estimated that 186 million people in the world have infertility issues. Infertility is defined as the inability to achieve conception by natural means through unprotectected sexual intercouse after one year. Gynaecologists, andrologists, nurses and psychologists are the professionals who attend to couples from the very beginning. However, there are also other important professionals in fertility centres who work discreetly and with no direct contact with patients, and yet help them in their aspiration to raise a family. They are mainly biologists, but there are also chemists or biotechnologists whose role inside the laboratory is crucial. The present text intends to explain more accurately who embryologists are, with details on their specific tasks in the laboratory. WHO ARE THE EMBRYOLOGISTS? An embryologist is a reproduction biology specialist. In particular, clinical embryologists are in charge of manipulating eggs, sperm and embryos in order to achieve fertilisation. Although most of the decisions related to treatments are often taken by doctors, it is the embryologists' call to decide on several aspects of the appropriate approach for the specific treatment (1), as well as coordinating the performance of every activity in the laboratory. In some countries, embryologists are even responsible for informing patients about certain laboratory procedures and, to some extent, embryo development, too (1). These responsibilities require embryologists to have wide experience in clinics, high degree of technical skills and extensive knowledge of reproductive human biology (2). TREATMENTS IN ASSISTED REPRODUCTION CLINICS Couples who decide to go through a fertility treatment are normally asked for blood tests to determine their hormone profile. Men usually go through semen analyses, too, and it is not uncommon for both partners to be subjected to physical examination if required, looking to discard specific abnormalities of the reproductive system. Once gynaecologists and/or andrologists have diagnosed the specific issue, they deliberate along with the senior embryologist on the most appropriate treatment depending on woman age, sperm quality or genetic problems. Broadly speaking, three different approaches can be considered: intrauterine insemination, in vitro fertilization and intracytoplasmatic sperm injection. Intrauterine insemination (IUI) is probably the easiest and least invasive procedure. It is indicated in very clear and specific cases such as tube obstruction, cervical factor infertility (3) or erectile dysfunction, and even some other unclear fertility issues that result in the inability to conceive by natural means (3). IUI consists in increasing gamete (spermatozoa) density at the site of fertilization by introducing sperm directly into the uterus (4). This technique requires previous sperm capacitation in the laboratory; capacitation is a natural process that comprises several physiological changes in the sperm necessary for fertilisation. Embryologists perform different procedures based on their evaluation of motile sperm that allows for selection of the best gametes (5) [find more about sperm selection in our previous post here]. Couples suffering from low sperm count or low sperm motility on the male side, or damaged Fallopian tubes or endometriosis on the female side (and more complex cases of infertility for either of them) are usually recommended to resort to either in vitro fertilization (IVF) or intracytoplasmatic sperm injection (ICSI) (depending on the particular situation). In both cases, ovarian stimulation is required for women. Hormonal stimulation of the ovary aims to increase the number of oocytes produced during the cycle; these oocytes must reach a minimum size in order to mature and be retrieved for the following procedures (either IVF or ICSI) (6, 7). Collection of oocytes is done through follicular puncture by means of laparoscopic transvaginal surgery. Whereas for IVF the sperm concentration used is similar to natural conditions in order to mimic the natural environment of the oocyte in the Fallopian tubes, cases of severe male factor infertility may require the use of ICSI (8). This procedure consists in the injection of an individual spermatozoon into the mature oocyte, thus being actually fertilised by the embryologist, one by one (9). Sperm selection is based on morphology and motility [learn more about sperm selection through our previous post here]. Twenty-four hours after the procedure, embryologists verify whether fertilisation has occurred by looking for two pronuclei under the microscope. The presence of two pronuclei is the first sign of fertilisation (one from each gamete), and they are to be fused into a single one in a process called syngamy (10). In some cases, fertile couples with genetic family history attend clinics in order to avoid passing the disease down to their offspring. Such situation requires performing preimplantation genetic diagnosis (PGD). This analysis, usually carried out at day 3 or 5 of embryo development, identifies embryos affected with the genetic disorder (11). Before being transferred, embryos are cultured for 3, 5 or 6 days (depending on a variety of factors and upon the embryologist´s own criterion). Based on PGD results, only healthy embryos will be selected for transfer into the womb. The number of embryos to be transferred is determined by specific regulations in each country, being just one the ideal situation, whereas spare embryos are derived for cryopreservation. Once all the above is done, the extensive work of the embryologist normally gets to an end. It is important to highlight that every single procedure is carried out in the laboratory under strict hygienic and sterile conditions. Also, the use of any perfume, deodorant and alike is completely forbidden just to prevent potential volatile organic compounds (VOS) from affecting developing embryos. In the laboratory, the use of caps, masks and the appropriate scrubs is mandatory for embryologists, and embryos are quickly placed in incubators that mimic the natural environment of the uterus (12). As for the timelines, embryologists work in shifts with the purpose of being available twenty-four hours a day, seven days a week. Assisted reproduction treatments must follow a strict timeline given the fact that procedures must be done at an exact time point in order to guarantee their success until transfer day. As a consequence, the work of embryologists is intense and often requires long-hour shifts. CONCLUSIONS Embryologists are extensively-trained professionals with wide experience in assisted reproduction technologies (ART) (1). To increase their knowledge and technical skills to perform ART-related procedures, they are continually trained in new methodologies and go through continuous education in the field of embryology (2). These highly-qualified professionals are in charge of the routine maintenance of the laboratory and equipment, sperm handling and processing for IUI, IVF and ICSI, cryopreservation of biological material, tissue sampling for biopsies for genetic analyses and PGD, or even embryo culture, among other tasks (2). These also include a strict and exhaustive record of the procedures for safety purposes. It is actually on the embryologists how to evaluate gametes and embryos, and to choose which ones are the most appropriate to be used and which should be kept in case future use is needed. It is without question that embryologists work tirelessly to help families achieve their dream of bringing a healthy baby home. REFERENCES
1-Medicine ASiR. The Alpha Consensus Meeting on the professional status of the clinical embryologist: proceedings of an expert meeting. Reprod Biomed Online. 2015;30(5):451-61. 2-Go KJ. 'By the work, one knows the workman': the practice and profession of the embryologist and its translation to quality in the embryology laboratory. Reprod Biomed Online. 2015;31(4):449-58. 3-Allen, N. C., Herbert, C. M., Maxson, W. S., Rogers, B. J., Diamond, M. P., & Wentz, A. C. (1985). Intrauterine insemination: A critical review. Fertility and Sterility, 44(5), 569-580. 4-Ombelet W, Van Robays J. Artificial insemination history: hurdles and milestones. Facts Views Vis Obgyn. 2015;7(2):137-43. 5-Fraser LR. Sperm capacitation and the acrosome reaction. Hum Reprod. 1998;13 Suppl 1:9-19. 6-Brinsden PR. Superovulation strategies in assisted conception. In: Brinsden PR. A Textbook of In Vitro Fertilization and Assisted Reproduction: The Bourn Hall Guide to Clinical and Laboratory Practice. Cambridge: Taylor and Francis group; 2005. p. 177-188. 7-Ventura-Juncá P, Irarrázaval I, Rolle AJ, Gutiérrez JI, Moreno RD, Santos MJ. In vitro fertilization (IVF) in mammals: epigenetic and developmental alterations. Scientific and bioethical implications for IVF in humans. Biol Res. 2015;48:68. 8-Eftekhar M, Mohammadian F, Yousefnejad F, Molaei B, Aflatoonian A. Comparison of conventional IVF versus ICSI in non-male factor, normoresponder patients. Iran J Reprod Med. 2012;10(2):131-6. 9-Simopoulou M, Gkoles L, Bakas P, Giannelou P, Kalampokas T, Pantos K, et al. Improving ICSI: A review from the spermatozoon perspective. Syst Biol Reprod Med. 2016;62(6):359-71. 10-Elder K, Dale B. Sperm-oocyte interaction. In: In-Vitro Fertilization. New York: Cambridge University Press; 2011. p. 50-63. 11-Beyer CE, Willats E. Natural selection between day 3 and day 5/6 PGD embryos in couples with reciprocal or Robertsonian translocations. J Assist Reprod Genet. 2017;34(11):1483-92. 12-Agarwal N, Chattopadhyay R, Ghosh S, Bhoumik A, Goswami SK, Chakravarty B. Volatile organic compounds and good laboratory practices in the in vitro fertilization laboratory: the important parameters for successful outcome in extended culture. J Assist Reprod Genet. 2017;34(8):999-100.
0 Comments
Leave a Reply. |
Categories
All
 2016-2019. All Rights Reserved by Embryologist Media. This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License . |
Embryologist Media